Introduction:
Fatty liver disease, particularly non-alcoholic steatohepatitis (NASH), is emerging as a silent epidemic with alarming prevalence rates worldwide. In India, it’s even more prevalent, with a prevalence of 38.7%, significantly higher than the global average of 27%. This case study by Dr. Sandeep Bhasin demonstrates a successful Grade 3 fatty liver reversal, where a 21-year-old patient showed remarkable improvement through a comprehensive, integrated treatment plan.
Shockingly, over half of diabetic individuals in India, standing at 58.7%, suffer from NASH. Even more concerning is the fact that young children are not immune, with a 35% incidence rate. In this article, we delve into the pressing issue of fatty liver disease and its implications, shedding light on the urgency of addressing this health crisis.
Fatty liver from NASH to MAFLD: a silent epidemic—Understanding fatty liver, diagnosing & managing with lifestyle modification, diet medications & intravenous protocols.
By Dr. Sandeep Bhasin
High Prevalence of NAFLD in India: Statistics and Impact
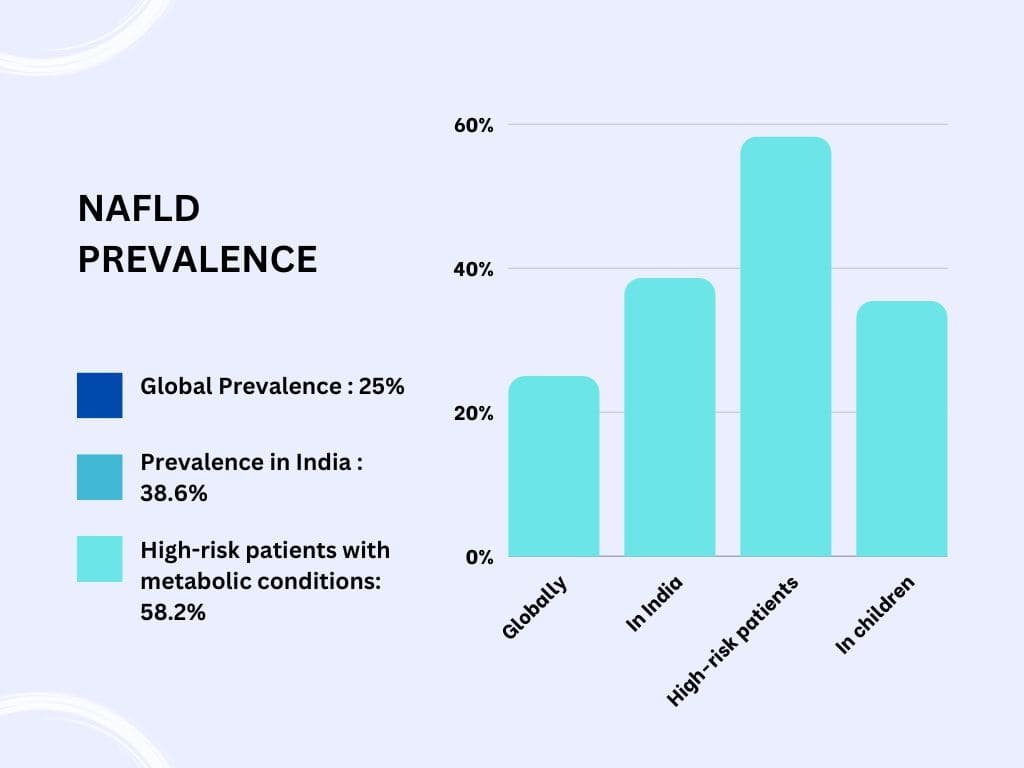
The prevalence of NAFLD is significantly high in India:
- Globally: 25%
- In India: 38.6%
- Among high-risk patients with metabolic conditions: 58.2%
- In children: 35.4%
Fatty Liver: A Silent Precursor to Health Crises

Many times, we don’t realize the hidden dangers of fatty liver, often brushing it off as a common issue in urban areas. What we need to understand is that NASH (Nonalcoholic Steatohepatitis) serves as a precursor to serious health conditions like liver fibrosis, cirrhosis, and even liver cancer. Highlighting the importance of early intervention, this case of Grade 3 fatty liver reversal proves that timely, integrated care can truly change the course of the disease:
- Diabetes
- Heart Diseases
- Cancer
- PCOD (Polycystic Ovary Syndrome)
- Infertility
- Fatigue
- Depression
- Sleep Apnea
- Kidney Disorders
- A leading cause of Liver Failure, surpassing Alcoholic Liver Disease, Hepatitis, and autoimmune disorders
If we don’t address this epidemic promptly, it could lead to a major health crisis in the near future.
Understanding NASH Diagnosis:
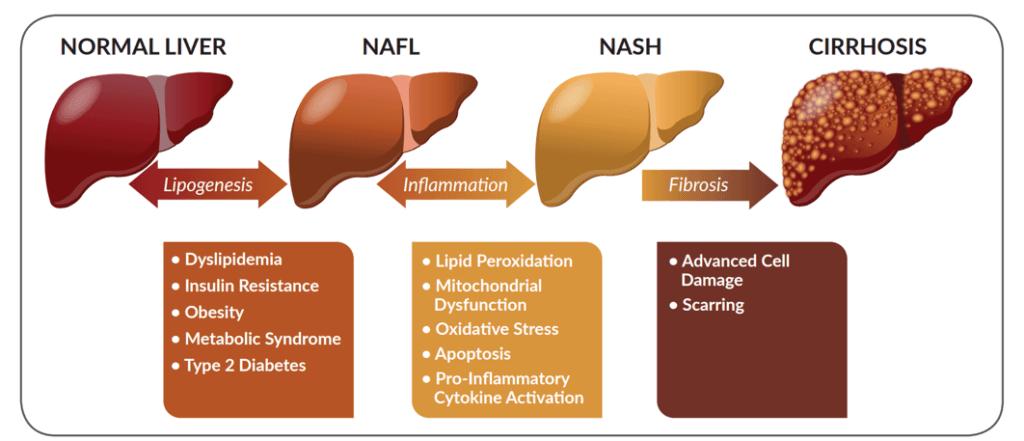
In simple terms, non-alcoholic steatohepatitis (NASH) is diagnosed when more than 5% of your liver is filled with fat. If you’re experiencing vague symptoms like fatigue, tiredness, weight gain, or discomfort in the upper abdomen, it’s a signal to be cautious. Doctors often use blood tests (Liver Function Tests or LFT) to check for elevated liver enzymes. An ultrasound of the abdomen can reveal a liver that looks brighter than usual (increased echogenicity). Let’s delve into these tests and what their results mean for your liver health:
- Specialized liver test: Fibroscan measures liver stiffness, and the Controlled Attenuation Parameter (CAP) measures liver fat.
- Healthy liver values: Ideally, liver stiffness should be below 7.5 kilopascals, and CAP should be under 225 decibels per meter.
- Fatty liver classification: Doctors classify fatty liver into three grades based on CAP values:
- Grade 1: CAP 225-250 Db/m
- Grade 2: CAP 250-275 Db/m
- Grade 3: CAP > 275 Db/m
With the ideal values in mind and the grades defined, these tests aid doctors in diagnosing and managing fatty liver disease effectively.
Case Presentation:
Under the care of Dr. Sandeep Bhasin, a 21-year-old nonalcoholic individual presented with symptoms such as fatigue, excessive weight gain, and overall tiredness. At the time of presentation, he had a weight of 105 kg and a BMI of 31.4. Routine blood investigations and an abdominal ultrasound were conducted, revealing elevated liver enzymes, a serum creatinine level of 1.4, an HbA1c of 6.5, and a homocysteine level of 30. Additionally, his HOMAIR was 2.8, CRP stood at 4.84, blood pressure measured 140/90, and his resting heart rate was 100. Fibroscan results indicated a CAP of 277 dB/m and a stiffness measure of 6.5, confirming Grade 3 fatty liver (NASH).
Treatment Approach:
Dr. Sandeep Bhasin took the time to educate the young and receptive patient about the diagnosis, potential complications, and the underlying causes of fatty liver. The emphasis was on the importance of lifestyle changes. The patient’s diet shifted towards plant-based options, minimizing non-vegetarian foods. He was allowed 2–3 eggs with salads, including the yolk, while reducing gluten and dairy intake to a minimum. Dr. Sandeep Bhasin’s treatment strategy for achieving Grade 3 fatty liver reversal focused on primarily targeting a 10% reduction in body weight. This approach involved a holistic, integrated plan:
- Patient Education: Dr. Sandeep Bhasin thoroughly informed the patient about his diagnosis, potential complications, and the pathophysiology of fatty liver. Understanding the importance of lifestyle modification was crucial.
- Dietary Changes: A plant-based diet was recommended, with minimal consumption of non-vegetarian foods. Eggs, including the yolk, were allowed, while gluten and dairy intake were minimized. Millets replaced wheat, and meals included salads with boiled eggs, protein shakes, lentils, kefir, and seasonal vegetables. Time-restricted eating and intermittent fasting were introduced, with an eating window between 12 noon to 7 p.m.
- Exercise and Stress Reduction: The patient was encouraged to engage in daily high-intensity interval training (HIIT) exercises, mindfulness meditation, and box breathing to manage stress effectively.
- Medications: Medications like Sarogltazar and Metformin were prescribed by Dr. Sandeep Bhasin to reduce insulin resistance. Nutraceutical supplements, including N-acetyl cysteine, alpha-lipoic acid, tocotrienol (a superior form of vitamin E), milk thistle, and vitamin D, were included in the treatment plan.
- Intravenous Therapy: The patient underwent intravenous treatments, including ozone saline, multivitamin drips, intravenous phosphatidylcholine, and alpha-lipoic acid.
Learn more about preventing and treating fatty liver in our comprehensive guide.
Outcome:
Under the care and direction of Dr. Sandeep Bhasin, the patient lost 15 kg of weight in 45 days. His energy levels went up a lot, and he became very driven to make the changes he was told to make. Over the course of 2 months, his clinical parameters demonstrated remarkable improvements:
Before Results
- Heart rate – 100
- Homocysteine – 30
- Serum Creatinine – 1.4
- Fibrosis – 6.5
- Fat Score – 277
- Weight – 105
- Homma IR -2.8
- CRP – 4.84
- BP – 140/90
After Results
- heart rate – 74
- Homocysteine – 14
- Serum Creatinine – .9
- Fibrosis – 5.8
- Fat Score – 227
- Weight – 90
- Homma IR – 1.5
- CRP – 1.5
- BP – 120/75

45 Days Before and After Result Photo
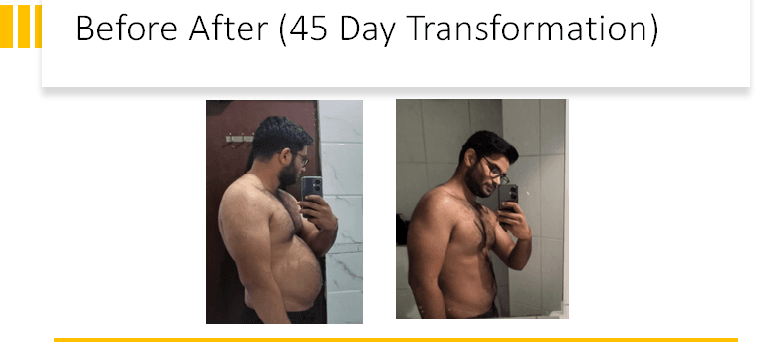
Conclusion:
Dr. Sandeep Bhasin’s case study highlights the significant correlation between fatty liver and insulin resistance. It shows how effective a complete method is, which includes changing your lifestyle, cutting back on carbs and calories, intermittent fasting, frequent exercise, stress management, specific medicines, and nutritional support. Grade 3 fatty liver reversal is possible when addressed early, helping prevent irreversible damage and leading to successful recovery.
Note: Please remember that this case study is only for your reference and to help you learn. Cases can be different, so it’s important to talk to a medical professional like Dr. Sandeep Bhasin to get specific help and care.










